D CEO Healthcare
The Business of Healthcare in North Texas
Healthcare
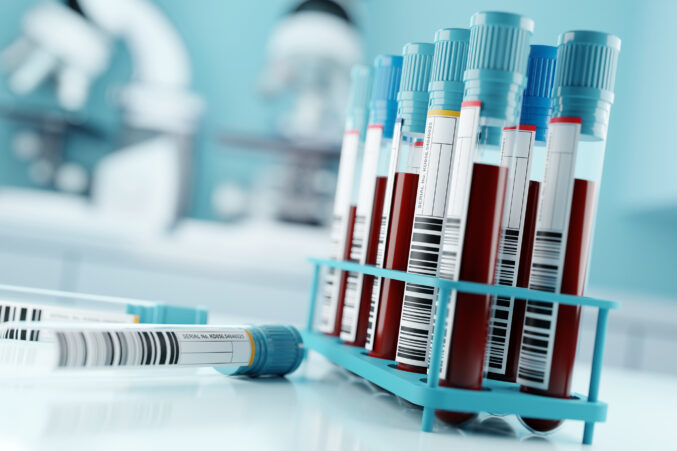
Dallas’ Breakthrough Blood Test for Cancer
With just 40ml of blood, Cancer Check Labs can test for the presence of more than 200 solid tumors.
By Will Maddox
Advertisement
Trending
Advertisement
Latest

Healthcare
Steward Health Files for Bankruptcy
Steward CEO Dr. Ralph de la Torre blamed government payers and other factors for the financial duress. The system owes top creditors $600 million.
By Will Maddox

Healthcare
Baylor Scott & White Waxahachie’s $240 Million Expansion
The medical center is growing to address a 40+ percent patient increase in the last five years.
By Will Maddox

Healthcare
Dallas Home Health Company to Pay $4.7 Million to Settle False Claims Allegations
A whistleblower was fired immediately after expressing concerns about improper payments from Medicare for patients who didn't qualify for hospice care at Elara Caring.
By Will Maddox
Healthcare
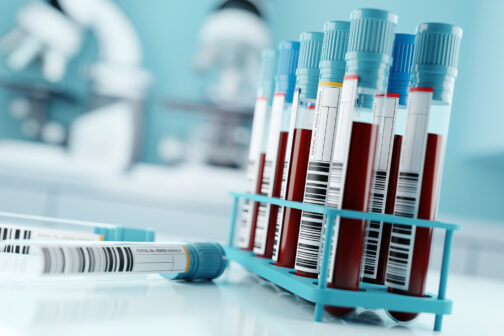
Dallas’ Breakthrough Blood Test for Cancer
With just 40ml of blood, Cancer Check Labs can test for the presence of more than 200 solid tumors.
By Will Maddox

News
Medical City Opens ER in Garland and Local Dermatologist Named Youngest Ever President of the American Academy of Dermatology
Plus Health Wildcatters wins accelerator competition and DFW Hospital Council Foundation awards.
By Bridget Reis
Advertisement
Latest
Healthcare
Local Physicians Say Cigna Owes Them Thousands and “Will Not Stand By” With Inaction
Leaders and physicians at Patient Physician Network say a change in the fee schedule has left them short on reimbursements for months.
By Will Maddox

Commercial Real Estate
What’s Behind DFW’s Outpatient Building Squeeze?
High costs and high demand have tenants looking in increasingly creative places.
By Will Maddox
Business
Why Wellness Brand Neora’s Victory May Not Be Good News for Other Multilevel Marketers
The ruling was the first victory for the multilevel marketing industry against the FTC since the 1970s, but may spell trouble for other direct sales companies.
By Will Maddox

News
Methodist Charlton Names New CEO and Steward Offloads Five More Hospitals for $1.1 Billion
Plus Texas Health Mansfield's new president and CEO, TimelyCare recognized by EY, and more.
By Bridget Reis

Healthcare
North Texas Healthcare Compensation: Who’s On Top?
Executives at Tenet Healthcare, McKesson Corp., and CHRISTUS Health lead the way.
By Will Maddox

